What if we told you that you can drive your organization’s health care costs down in a science-driven, sustainable way, while measurably improving employee health and well-being?
HealthPartners' Total Cost of Care (TCOC) approach is our solution to strategic, sustainable health and cost improvements. It’s one of only two third-party health care measurement frameworks endorsed by the National Quality Forum (NQF). The federal government, states and private-sector organizations across the United States use NQF-defined measures or health care practices as the best, evidence-based approaches to improving care.
TCOC takes an all-encompassing look at how health care is managed across conditions, providers, individual plan members and entire employee populations. Government entities, researchers, providers and employers have used it for over a decade to understand health care costs and create better care efficiencies.
As an integrated care delivery system and health insurance carrier, we use the TCOC analysis to capture, track and improve many of the myriad member touch-points and cost variations that affect the total health care expenditures of an employer’s population.
Why discounts are only part of the story
Before we dive into how TCOC can help, let’s examine the concept of discounts since we know they are top-of-mind for most employers.
“Discounts are only part of the story,” explains Chris Parrucci, HealthPartners Business Manager for Labor and Public Sector Accounts. “Other health plans may offer employers a 50 percent discount on a hospital stay, for example. That means an employer will pay a 50 percent discount within a fee schedule. But if HealthPartners can keep people healthier and prevent them from being admitted to a hospital in the first place – we just saved that organization and its members significantly more money than they'd get with a discount alone.”
There’s nothing wrong with focusing on discounts. Purchasers must be confident their vendor offers competitive discount pricing associated with their network. Yet, as Parrucci says, it’s better for your business in the longer term to focus on how your medical plan will help nudge your population towards better overall health and well-being, while avoiding more expensive, potentially less effective levels of care.
“It’s about providing the appropriate type of care and support when your employees need it, in a way that will work best for them as individuals. It's making sure you are providing the right care the first time,” adds Parrucci.
So, how does your organization move from simply comparing discounts towards providing employees with high-quality, affordable care that can measurably improve their health?
First, you have to understand more deeply how HealthPartners’ TCOC process can work for your organization.
TCOC process explained
Honing in on the hitches in health care
Here’s how it works. When we partner with employers, we analyze their historical health care claims, and look for cost variations and patterns of misuse from a standard or expected level of care in a similar population.
“TCOC is all about trying to understand what we are observing in people’s health journeys relative to what we would have expected and the “why” behind it,” says Jason Gallagher, Vice President of Health & Care Engagement at HealthPartners. “And through that analytical approach combined with clinical expertise, we identify opportunities for us to improve outcomes and change the approach.”
Being able to ascertain the why behind the variation is critical. For example, we ask questions like:
- Why do we see more back surgery in a population than conservative therapy approaches?
- Why are people choosing the emergency room instead of virtual care?
- Why are infusions happening in the hospital instead of in the home?
- What is unique about this provider’s care model that results in more testing and diagnostic imaging?
- And the list goes on…
”TCOC enables us to support members differently and partner in unique ways with network providers to make a difference,” adds Gallagher.
Right time, right care: Supporting members’ health care journeys
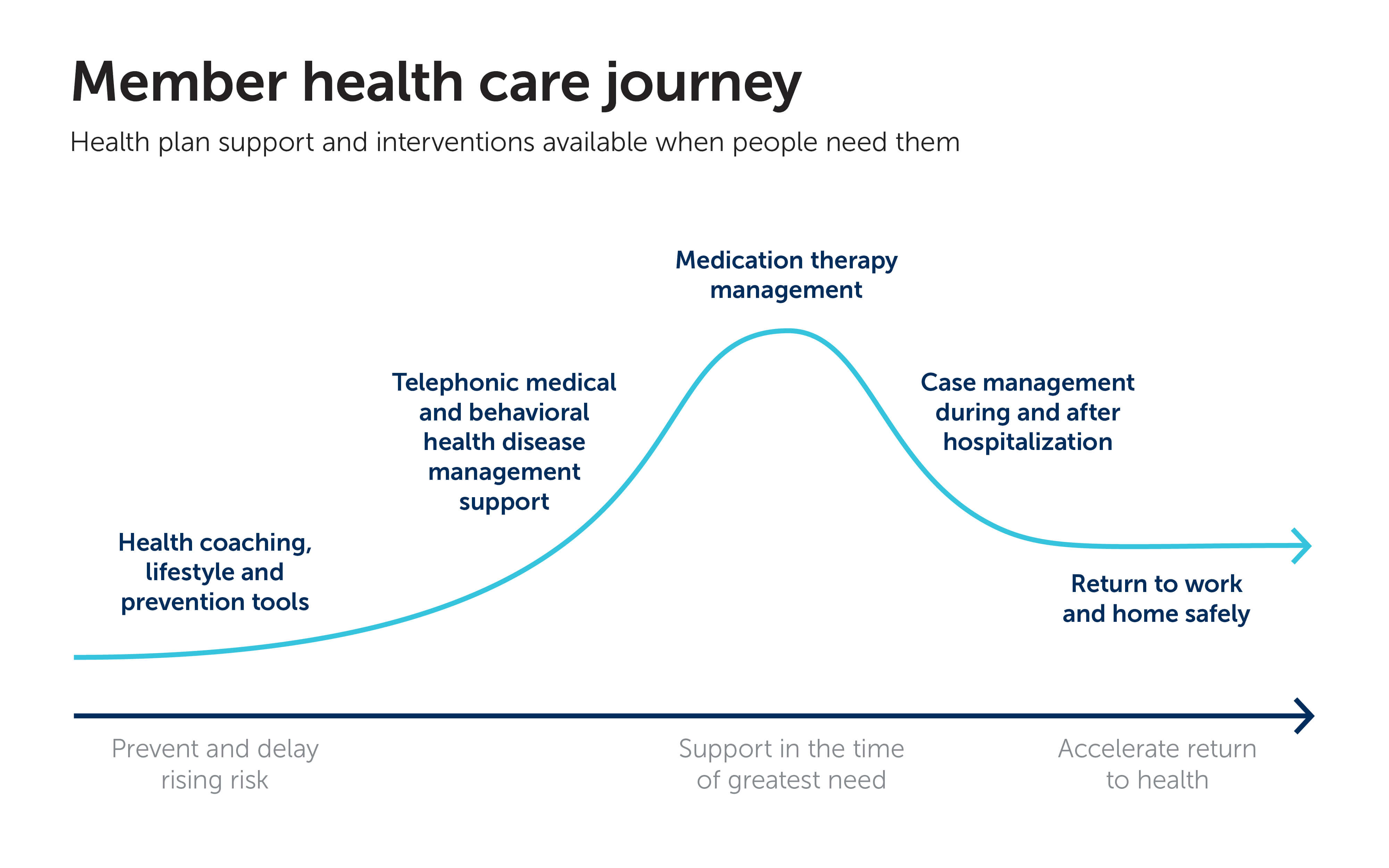
Supporting members on their personal health care journey is a key part of impacting the total cost of care. The care experience timeline [pictured], shows a generalization of every person’s health care needs and how they evolve over time. This curve holds true for a person who has a case of acute sinusitis where the duration is very short, and the needs small, culminating in a prescription and a quick recovery. It also holds true for a person with chronic low back pain, which lasts a long time, resulting in high cost surgery or an ongoing need of physical therapy.

It's a helpful way to visualize the moments when the right support and care are most crucial in both reducing the intensity and impact of a health issue and in speeding recovery.
“We can think about our TCOC approach in terms of changing the shape of this curve. By tackling health problems upstream, we impact the slope of that curve,” explains Gallagher. “By supporting people in the times that they need it the most, we reduce the magnitude and cost of their experience. And by helping people return to health as it could and should be, we change the duration of those experiences. That’s lowering the total cost of care.”
Here’s an example: If we consider the health journey for an employee with diabetes, we start building interventions and experiences that will engage the member and positively impact that journey. For example, we deploy pre-diabetes coaching to impact lifestyle choices. We use medication therapy management to optimize dosing of hypertension medications. We provide case management support before, during and after a hospitalization to help that person get safely home and back to work.
Discharge planning for hospital patients is a key opportunity to impact the health curve and reduce the likelihood of future health care episodes.
"We have care managers on-site when somebody is admitted with a HealthPartners insurance card. Care coordination is happening between the hospital’s physicians, for example, and our disease case managers,” explains Parrucci. “Our case managers ensure proper discharge planning to prevent re-admission.”
Each of those interventions, timed and curated into an experience, impacts the health care journey for an individual. This approach, deployed across a population, impacts the total cost of care for an organization.
Partnering with providers to raise the bar on care
Another key part of TCOC is close collaboration with care providers across care systems to understand in depth how they are performing and and help them improve.
“We work with providers to ensure they are meeting goals around cost and quality. We have long-term, excellent collaboration, frequently sharing the latest clinical research from our HealthPartners Institute. Other insurance carriers often fail or fall short because it's difficult to manage," Parrucci explains.
The aim is to support collaboration between providers and shared accountability for success through, for example, care delivery enhancements, smart referrals, and early adoption of innovations.
The strategy is three prong:
- Improve population health through clinical outcomes
- Create an exceptional experience for the individual
- Examine ways to create affordability and shared savings through improved care delivery treatment models.
“TCOC is a powerful tool for identifying both best practices, where things are working well, and opportunities to improve outcomes at scale,” says Gallagher. “At the consulting level, whether with employers, providers, or government regulators, we can then discuss cost variation in their particular population and improvement strategies.”
TCOC savings in action
The following analysis summarizes our work with two trade unions - the Bricklayers & Allied Craftworks and the Cement Masons using our TCOC solution.
Beginning with a three-year analysis of claims prior to moving to HealthPartners, the TCOC approach helped each union identify practical ways to reduce costs and support employee health and well-being. These included:
- High-performing provider networks that effectively coordinate the appropriate care, delivering market-leading outcomes at an affordable cost
- Health and care engagement programs that leverage technology and evidence-based best practices to engage members and measurably improve health
- Medical claims, pharmacy claims and internal plan administration management that streamlines efficiencies and costs.
“We looked at everything, not just the design of their network, but the back-end management of their claims, admin fees, and provider relationships to see where costs could be reduced. We can do that effectively because we are an integrated health insurance and care delivery organization,” explains Parrucci. “No other carrier works with providers in this way.”
Three years after making the move to HealthPartners, the Bricklayers and the Cement Masons each experienced over 12 percent in cost savings while also seeing a significant increase in the number of members enrolled in their medical plans.
“We definitely saved money with HealthPartners’ cost guarantee,” adds Doug Schroeder, President and Secretary/Treasurer of the Bricklayers & Allied Craftworks. “We’ve seen success with people living with diabetes through HealthPartners’ disease management program. It’s more seamless for members to participate, and the process is simpler and quicker, especially with the apps. We’ve also experienced a better-executed claims process.”
